Hip arthroscopy has become a popular procedure over the last few years, registering a growth of over 250 percent from 2007 to 2011.
The hip is a highly constrained joint, having thick soft tissue envelope, it becomes necessary to create distraction of the joint in order to visualize the central compartment for surgery.
To access the hip joint during arthroscopy, a traction table is typically used with a perineal post to allow for counter-traction and achieve hip distraction. A traction force of 89 to 127 lb may be required to adequately distract the joint in anesthetized patients.
The perineal post causes high force vectors against the patient’s groin, leading to two different traction complications (associated directly with the perineal post). These include:
- Pressure-related soft tissue damage to the perineum
- Compression-related neurapraxias and permanent injury to the pudendal and other surrounding nerves
Assessing the Safety of a Postless technique
A scientific study was performed to prospectively assess the safety of a postless technique for hip distraction during hip arthroscopy. During the course of the study, a total of 1000 hip arthroscopies were performed, and no groin related soft tissue or nerve complications took place.
The study also found no complications (friction burns, skin contusions) as a result of the necessary friction created between the patient’s body and the operating table.
630 subjects were evaluated for a follow-up at two years after surgery, and another 270 were evaluated after at least one year post-operatively as part of the study.
Challenges of Using a Perineal Post
Most patients undergoing hip arthroscopy are young, athletic, and sexually active. Furthermore, hip arthroscopy is an elective procedure. Therefore, perineal nerve- and soft tissue-related complications should be considered unacceptable in this population undergoing this procedure.
With the use of a perineal post, the largest barrier for new hip arthroscopists as well as the most significant concern for experienced surgeons is not the procedure itself but rather the potential complications that may arise based on patient positioning.
Benefits of a Postless Technique
In addition to eliminating nerve and soft tissue related complications, the use of the postless technique for hip arthroscopy offers several other benefits.
In particular, for new hip surgeons who need more time to enter the joint and work in the central compartment, the post-free technique minimizes concerns of complications that may become evident postoperatively. Therefore, this technique allows surgeons to focus on the procedure itself rather than the complications that may occur with the use of a traction post.
Another benefit, which allows the surgeon to enter the joint safely and reproducibly, is the ability to use anteroposterior and true lateral fluoroscopy views when positioning the first needle while establishing the first portal.
An additional advantage possibly affects the anesthetic and surgical fronts, and this is improved blood return to the heart and brain perfusion attributed to the inclined position, which may make it easier to control and maintain a lower blood pressure, thereby enabling the use of lower pump pressure.
Finally, the ability to perform bilateral hip arthroscopy under the same anesthetic without accumulated groin-related stress and increased groin-related complications enables faster recovery for patients with bilateral disease.
Source: NIH
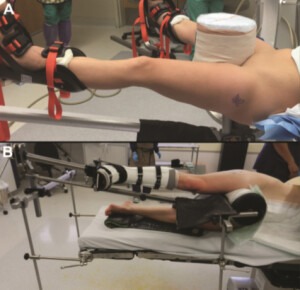
Intraoperative photograph demonstrating (A) supine and (B) lateral positioning for hip distraction utilizing a 10-inch perineal post. Both techniques achieve hip distraction by applying countertraction to the perineum.
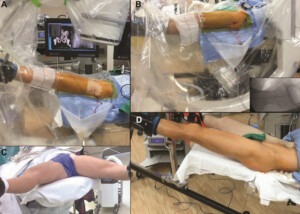
(A) Intraoperative photograph demonstrating technique for obtaining an anteroposterior fluoroscopic view by arcing the fluoroscope to maintain an orthogonal beam trajectory to the patient in Trendelenburg. (B) A cross-table lateral hip fluoroscopic view can be obtained by positioning the fluoroscope between the patient’s legs, with good visualization attributed to the absence of the perineal post. The fluoroscopic image demonstrates central placement of the 17-gauge, 6-inch needle utilized to percutaneously establish the midtrochanteric portal. (C, D) Intraoperative photographs of the postless technique showing no pressure on the perineum during application of traction
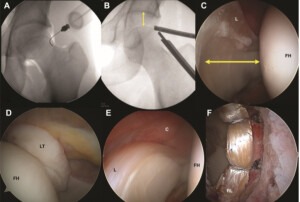
(A) Anteroposterior fluoroscopic image of a left hip before the application of traction with a 17-gauge, 6-inch needle placed intracapsularly at the level of the femoral head-neck junction to perform an air arthrogram. Air can be seen outlining the labrum laterally and demarcating the level of the zona orbicularis. (B) Gentle application of traction is performed after venting the joint with an air arthrogram, achieving the desired degree of distraction within the hip joint (arrows), as demonstrated in this posttraction anteroposterior fluoroscopic view of the left hip. (C) Arthroscopic view of a right hip with a 30 arthroscope placed in the midtrochanteric portal (the senior author’s version of the anterolateral portal) visualizing the femoral head (FH) to the right, the acetabulum and labrum (L) to the left, and adequate space for instrumentation in between (arrows). (D) Arthroscopic view of a left hip with a 70 arthroscope inserted through the midanterior portal deep into the central compartment to visualize the cotyloid fossa, ligamentum teres (LT), and inferomedial femoral head. (E) Arthroscopic view of a right hip with a 30 arthroscope inserted through the midtrochanteric portal visualizing the anterosuperior labrum, anterior capsule (C), and femoral head, or the so-called anterior triangle, before establishing the midanterior portal under direct visualization. (F) Arthroscopic view of a left hip with the 30 arthroscope placed through the midtrochanteric portal after a labral reconstruction showing the acetabular rim and wellpositioned reconstructed labral (RL) graft. All intraoperative visualization was achievable with postless distraction.
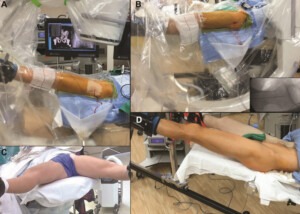
Intraoperative photographs showing (A) the use of a smartphone application to measure the degrees of Trendelenburg tilt on the operative bed before the application of traction; (B) the pressure transducer reading for measuring traction force throughout the procedure; and (C) the locking mechanism for the traction boot and the spider device as well as (D) the positioning of the limb in the traction boot.
Dr. Tigran Garabekyan is a board certified orthopedic surgeon specializing in hip preservation. To learn more about Southern California Hip Institute or to schedule a consultation, click here to contact us or call:
North Hollywood: 818.755.6500
Century City / Los Angeles: 310.595.1030
Serving patients in Encino, Sherman Oaks, Van Nuys, North Hollywood, Burbank, Glendale, West Hollywood, Century City, Beverly Hills, Santa Monica, Los Angeles, and other neighboring cities in the greater Los Angeles area.
Also visit http://www.drgorthopedics.com/